Fix What is Wrong
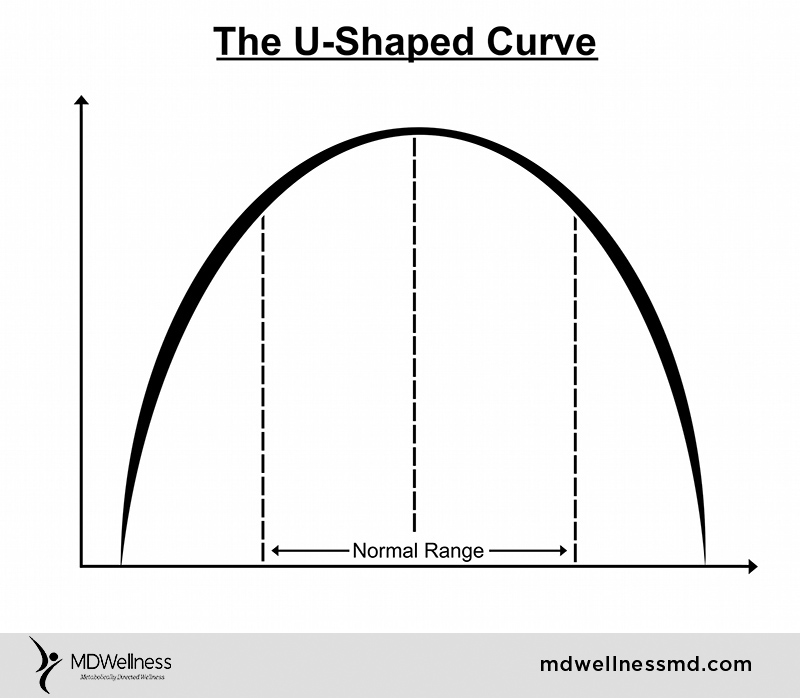


“Everybody knows” there are good fats and bad fats
Put a Log on the Fire
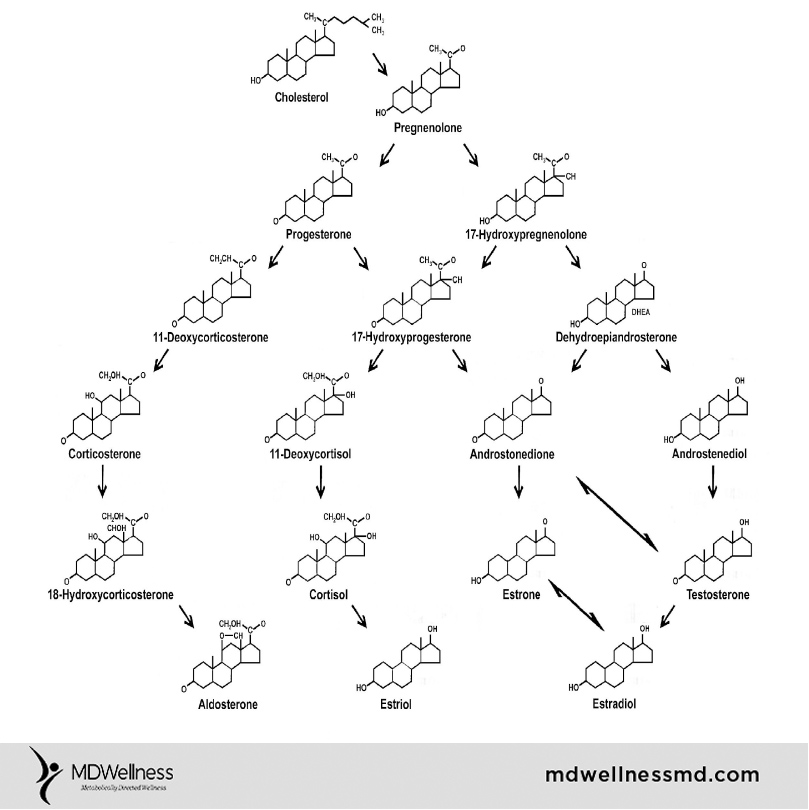
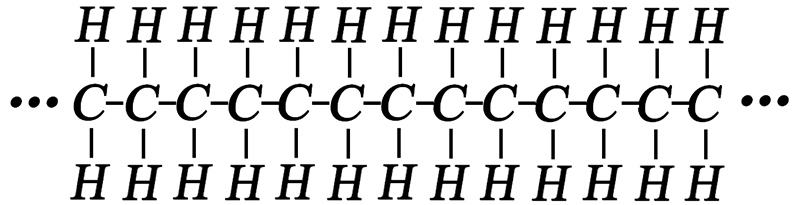
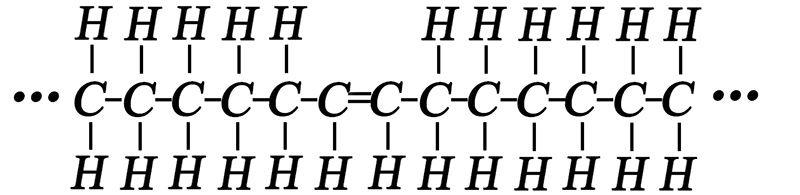


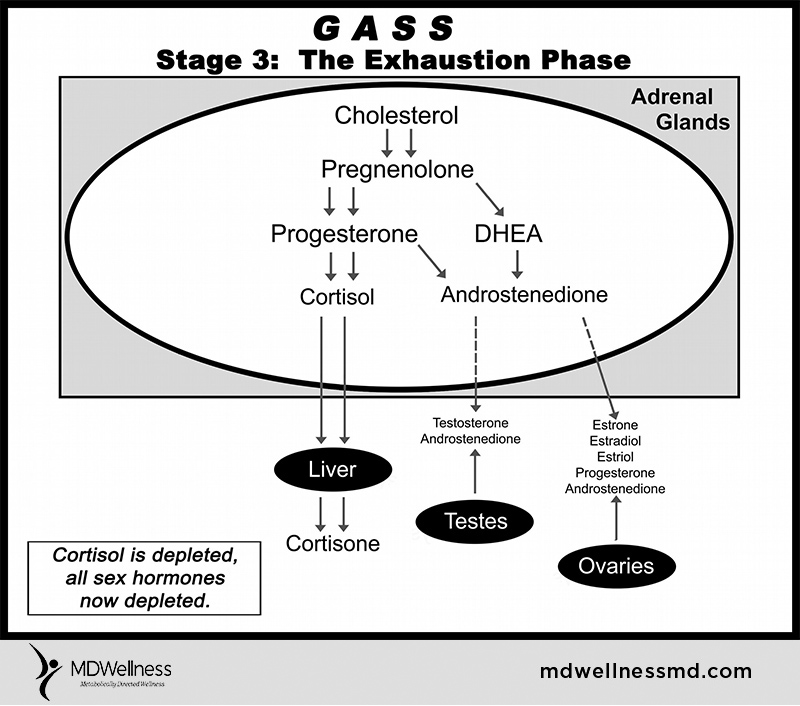


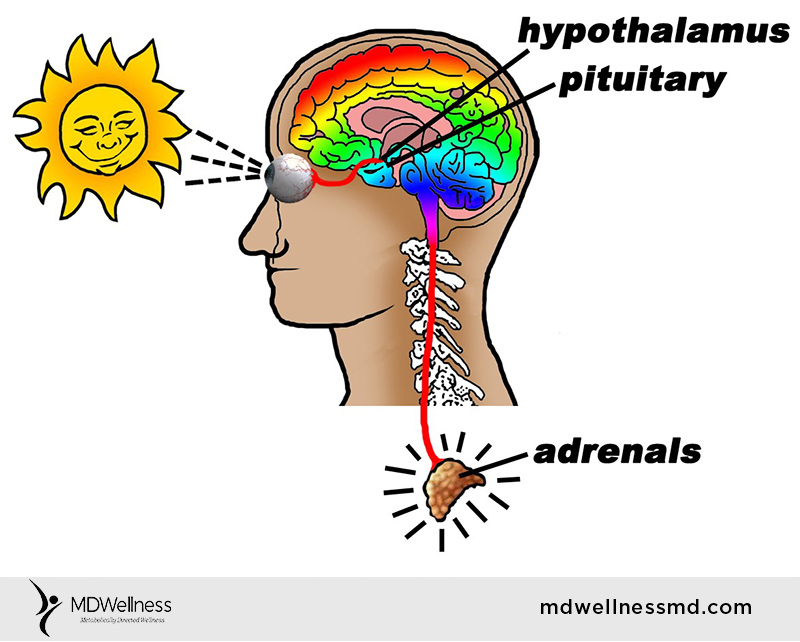
What is intermittent fasting?
What is a “non-fed” state?
Why is Insulin Resistance (IR) so detrimental to health?
Doesn’t a calorie-restricted diet do the same thing?
Transitioning to Intermittent Fasting
Tips for success
What Should I Eat?
Saturated Fats, Won’t They Hurt Me?
Meta-analysis of prospective cohort studies evaluating the
association of saturated fat with cardiovascular disease
Patty W Siri-Tarino, Qi Sun, Frank B Hu and Ronald M Krauss 1 From the Children’s Hospital Oakland Research Institute
Oakland CA Harvard School of Public Health Boston MA.
ABSTRACT
Background: A reduction in dietary saturated fat has generally been thought to improve cardiovascular health.
Objective: The objective of this meta-analysis was to summarize the evidence related to the association of dietary saturated fat with risk of coronary heart disease (CHD), stroke, and cardiovascular disease (CVD; CHD inclusive of stroke) in prospective epidemiologic studies.
Design: Twenty-one studies identified by searching MEDLINE and EMBASE databases and secondary referencing qualified for inclusion in this study. A random-effects model was used to derive composite relative risk estimates for CHD, stroke, and CVD.
Results: During 5–23 y of follow-up of 347,747 subjects, 11,006 developed CHD or stroke. Intake of saturated fat was not associated with an increased risk of CHD, stroke, or CVD. The pooled relative risk estimates that compared extreme quantiles of saturated fat intake were 1.07 (95% CI: 0.96, 1.19; P = 0.22) for CHD, 0.81 (95% CI: 0.62, 1.05; P = 0.11) for stroke, and 1.00 (95% CI: 0.89, 1.11; P = 0.95) for CVD. Consideration of age, sex, and study quality did not change the results.
Conclusions: A meta-analysis of prospective epidemiologic studies showed that there is no significant evidence for concluding that dietary saturated fat is associated with an increased risk of CHD or CVD. More data are needed to elucidate whether CVD risks are likely to be influenced by the specific nutrients used to replace saturated fat.
Harvard Medical School Published in the American
Journal of Clinical Nutrition January 2010
Breast Milk
Low Intake of Saturated Fat
Effect of low-fat diets on plasma high-density
lipoprotein concentrations
Katan MB.
Department of Human Nutrition, Wageningen Agricultural University, The Netherlands.
Low concentrations of HDLs in plasma are a strong predictor of risk for coronary as well as other cardiovascular diseases. There is increasing evidence that this relation is causal and that interventions that change HDL concentrations also change risk. One such intervention is exchanging fat and carbohydrate. In controlled trials, low-fat, high-carbohydrate diets decrease HDL concentrations. The effect is strongest when carbohydrates replace saturated fatty acids, but is also seen when carbohydrates replace mono- and polyunsaturated fatty acids carbohydrates. The effect is seen in both short- and long-term trials and therefore appears to be permanent. This finding is supported by epidemiologic studies in which populations eating low-fat, high-carbohydrate diets were shown to have low HDL concentrations. Weight losses with consumption of low-fat diets could theoretically counter effects on HDL, but in published trials weight losses have been modest and insufficient to offset the decrease in HDL concentrations induced by carbohydrates. Thus, replacement of saturated fat by carbohydrates adversely affects plasma HDL concentrations; replacement of saturated fat by unsaturated fatty acids deserves consideration as an alternative.
PMID: 9497172 [PubMed – indexed for MEDLINE]
American Journal of Clinical Nutrition
Metabolic Syndrome
High Carbohydrate Diets, Triglyceride Rich Lipoproteins,
and Coronary Heart Disease Risk
– American Journal of Cardiology 2000
Abbasi F, McLaughlin T, Lamendola C, Kim HS, Tanaka A, Wang T, Nakajima K, Reaven GM.
Stanford University School of Medicine, California, USA.
In this study we compared the effects of variations in dietary fat and carbohydrate (CHO) content on concentrations of triglyceride-rich lipoproteins in 8, healthy, nondiabetic volunteers. The diets contained, as a percentage of total calories, either 60% CHO, 25% fat, and 15% protein, or 40% CHO, 45% fat, and 15% protein. They were consumed in random order for 2 weeks, with a 2-week washout period in between. Measurements were obtained at the end of each dietary period of plasma triglyceride, cholesterol, low-density lipoprotein (LDL) cholesterol, high-density lipoprotein (HDL) cholesterol, remnant lipoprotein (RLP) cholesterol, and RLP triglyceride concentrations, both after an overnight fast and throughout an 8-hour period (8 A.M. to 4 P.M.) in response to breakfast and lunch. The 60% CHO diet resulted in higher (mean +/- SEM) fasting plasma triglycerides (206 +/- 50 vs 113 +/- 19 mg/dl, p = 0.03), RLP cholesterol (15 +/- 6 vs 6 +/- 1 mg/dl, p = 0.005), RLP triglyceride (56 +/- 25 vs 16 +/- 3 mg/dl, p = 0.003), and lower HDL cholesterol (39 +/- 3 vs 44 +/- 3 mg/dl, p = 0.003) concentrations, without any change in LDL cholesterol concentration. Furthermore, the changes in plasma triglyceride, RLP cholesterol, and RLP triglyceride persisted throughout the day in response to breakfast and lunch. These results indicate that the effects of lowfat diets on lipoprotein metabolism are not limited to higher fasting plasma triglyceride and lower HDL cholesterol concentrations, but also include a persistent elevation in RLPs. Given the atherogenic potential of these changes in lipoprotein metabolism, it seems appropriate to question the wisdom of recommending that all Americans should replace dietary saturated fat with CHO.
Manifestations of Low Saturated Fat Diet
Disclaimer: The information provided on this site is for educational purposes only and does not substitute for professional medical advice. Please consult a medical professional or healthcare provider for medical advice, diagnoses, or treatment. If you are experiencing a medical emergency, dial 911.
© 2024 Michael Rothman, LLC d/b/a Michael Rothman, MD. All rights reserved. | Privacy Policy | Terms & Conditions | Shipping & Return Policy
Website Created and Managed by M&A consulting
Schedule a Free Consult
Complete this quick form to schedule a
non-obligation 15 minutes phone consultation.